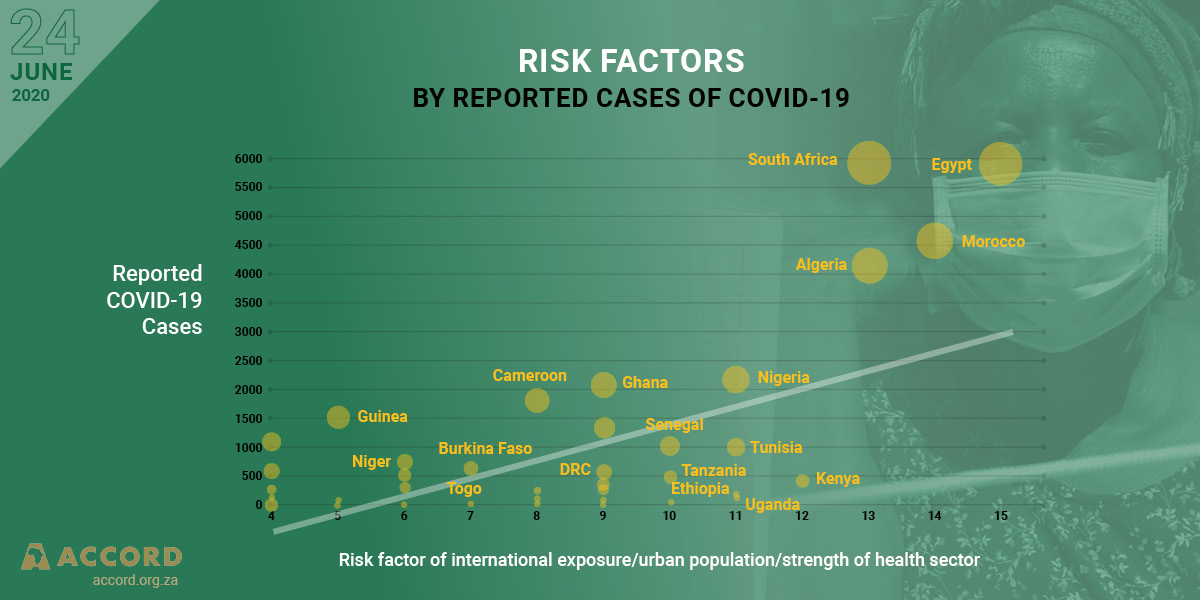
Meanwhile, the African continent is an outlier, with 17% of the world’s population but only accounting for 1.1% of COVID-19 cases and 0.7% of related deaths. While the wide geographic spread of the infection in Africa suggests a large number of unreported cases and deaths, overall, the number of infections remains low and does not follow the same pattern as its Asian and Western counterparts.
The spread of the virus in Africa is now starting to accelerate. The first 100,000 confirmed cases accumulated in 98 days, but it took only 18 days to reach 200,000.
Tweet
Why has the disease taken a different path in Africa?
According to the World Health Organization (WHO), a slower rate of transmission, lower age of people with severe disease and lower mortality rates have been observed in Africa, compared to the most affected countries in other parts of the world. The WHO says this is largely driven by social and environmental factors slowing the transmission, and a younger population that has benefited from the control of communicable diseases such as HIV and tuberculosis to reduce possible vulnerabilities.
Evidence has indicated that the elderly are the most affected by COVID-19. Africa has a much younger population than say, China, the European Union and the US. Only 3% of the region’s population is over the age of 65, which is the threshold for a significantly higher risk of COVID-19-related complications and death. The median age of Africa’s population is 19.4 years and 60% of the population is under the age of 25 years.
Researchers have drawn attention to the fact that in Europe and the US, the majority of the elderly live in retirement homes. In Sweden, care home residents account for nearly half of the deaths linked to COVID-19. Residents in old-age care facilities live in close proximity to each other, whereas in Africa many of the elderly live at home with their families, which may help protect this age demographic. However, researchers warn that since Africa’s youthful population is impacted by other diseases such as HIV and malnutrition, this may make them vulnerable to COVID-19.
Other causes that could explain the slow rate of infection in Africa that have been considered include warmer weather, a low population density, less travel and effective cross-border cooperation.
An important factor that is seldom mentioned is the way in which the disease has been managed in Africa to date. The slow onset, models emerging (particularly from China and Italy), lessons from earlier disease experiences such as Ebola and HIV, strong leadership from the African Union’s (AU) African Centres for Disease Control and Prevention (Africa CDC) and good cooperation with the WHO have enabled African countries to act early and decisively. Border closures, limitations on internal movements and strict social-distancing measures were introduced far sooner in Africa than other countries at similar infection levels.
The Bureau of the AU, ministers of health and the Peace and Security Council (PSC) met several times to coordinate the African response and to develop continental plans. Africa demanded and was successful in arranging debt relief. The AU created a COVID-19 Response Fund and the Partnership to Accelerate COVID-19 Testing (PACT), and plans are currently underway to ensure that Africa is sharing its COVID-19 lessons, joining forces when it comes to procuring essential materials, and cooperating in the development and spread of vaccines. By pooling expertise at the multilateral level, the AU has provided technical assistance to its member states, played a critical role in supporting coordination among them, and helped to mobilise support with international partners.
However, there are also other demographic and political factors in Africa that are of serious concern, and which could exacerbate the spread of the virus. In 2019, sub-Saharan Africa was host to more than 17 million internationally displaced persons (IDPs) and six million refugees – more than a quarter of the world’s refugee population. Africa is rapidly urbanising, but approximately 60–70% of people in cities are living in high-density areas with poor sanitation. In both slums and refugee and/or IDP camps, social distancing, frequent hand-washing and isolation may not be realistic. Eighty-five per cent of Africa’s forcibly displaced persons are concentrated in eight countries: the Democratic Republic of the Congo (DRC), South Sudan, Somalia, Ethiopia, Sudan, Nigeria, the Central African Republic (CAR) and Cameroon – all of which are countries affected by conflicts.
Another vector for spreading the disease is migration. Violent conflict, social unrest, climate change and economic opportunities have been drivers for migration in Africa in the past, and COVID-19 could become another driver. Approximately 24 million people in the Sahel will need life-saving assistance and protection as a result of the escalating violence taking place in the Sahel and West African region.
However, it is also important to bear in mind that many of the previous public health worst-case scenarios related to Ebola and the HIV/Aids epidemics have not materialised, partly because although governance is weak in some African countries, social and community resilience is generally robust.
Will Africa be the last epicentre of the virus?
Although many of the factors considered above may have contributed to slowing down the spread of the virus in Africa, it is now starting to accelerate. Whilst the continent registered its first 100 000 confirmed cases in 98 days, it took only 18 days to reach 200 000 cases, and it may take only half as many cases again to reach 300 000 cases. “Even though these cases in Africa account for less than 3% of the global total, it’s clear that the pandemic is accelerating,” WHO Africa head, Matshidiso Moeti, confirmed at a media briefing.
Director of the Africa CDC, John N. Nkengasong, and co-authors warn in a paper published in Nature Medicine that given the current trends in incidents and underlying healthcare systems vulnerabilities, Africa could become the next epicentre of the COVID-19 pandemic. Accordingly, there are fears that with Africa’s high levels of poverty, weak health systems and crowded urban areas, the virus could be particularly devastating on the continent. These dire predictions have not come to pass, but if the disease continues to spread at its current rate, the situation in Africa could become much worse.
To date, the measures introduced to contain the spread of COVID-19 have had a greater impact on the everyday lives of most people on the continent than the virus itself. This may change when the overall number of infections starts to increase significantly. Although the measures taken to date have allowed many countries the time to prepare for the peak of the virus and to scale up their capacity, especially within the health sector, a high caseload of patients who need medical care is likely to eventually overwhelm Africa’s limited health systems. These effects in the health sector, together with measures to stem the virus, will expose and compound pre-existing social, political and economic fault lines, especially in conflict-affected countries and regions, and stress-test social cohesion and resilience.